Some Different Perspectives On Methylene Blue
Maybe Not As Good For You As Some Claim
I tried Methylene Blue once and did not feel good afterwards. Have avoided it since. I think Alex Jones has gotten this wrong.
Three Articles Follow: Two from Sayer Ji’s Substack and then an important article by Dr. Peter Breggin from his substack:
4
The Blue Brain Effect: Methylene Blue’s Dark Side & What You Should Be Using Instead
Biohackers are turning to methylene blue—but what exactly is this synthetic, petroleum-derived chemical doing to the human body, and at what cost?
Mar 09, 2025
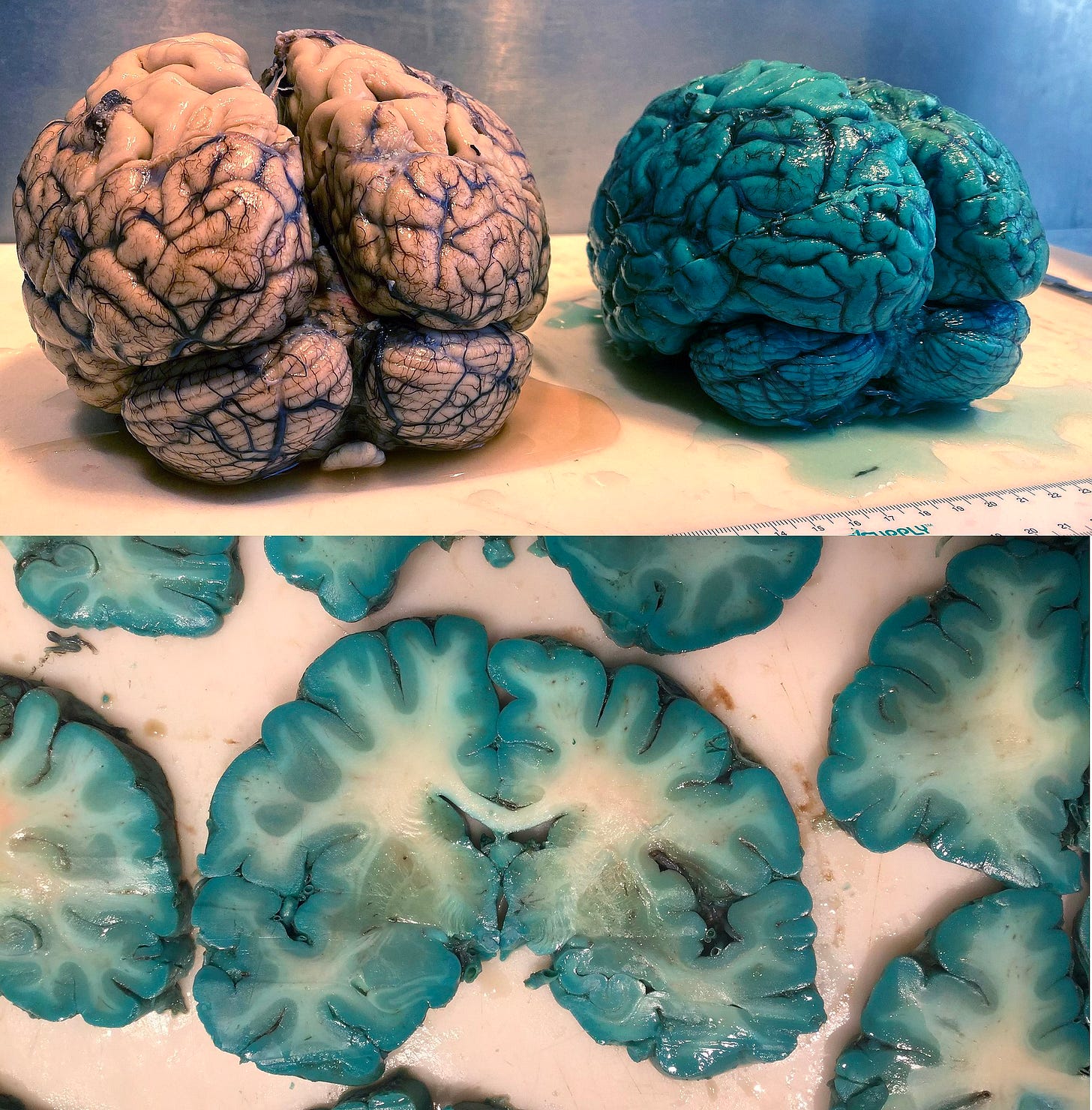
If this is what methylene blue in the brain post-mortem looks like, what is it doing while you're alive?
A recent study published in Forensic Science, Medicine and Pathology titled, “Fifty shades of green and blue: autopsy findings after administration of xenobiotics” has brought to light striking findings regarding methylene blue's impact on our internal organs. The research documented cases where systemic administration of methylene blue resulted in a pronounced blue-green discoloration of various organs, notably the brain and heart.
This discoloration is attributed to methylene blue's strong affinity for biological tissues, leading to its accumulation and subsequent staining. The study's observations raise critical questions about the compound's interactions within the human body, especially concerning its potential to cross the blood-brain barrier and the implications of its presence in neural tissues.
While methylene blue has been employed therapeutically within the allopathic medical context for various conditions, these findings underscore the necessity for a deeper understanding of its biodistribution and long-term effects on organ systems, particularly the brain. The visible staining observed post-mortem prompts further investigation into whether such accumulation has functional consequences during a patient's life, emphasizing the need for comprehensive safety evaluations.
Methylene Blue: A Century-Old Medical Staple Under New Scrutiny
In hospitals and medical facilities worldwide, a vibrant blue liquid flows through IV tubes into patients' veins, stains surgical sites, and colors diagnostic tests. This substance is methylene blue (MB)—a synthetic compound that has been used in medicine for over a century. While touted as a treatment for conditions ranging from malaria to circulatory shock, emerging research suggests it's time to reassess our understanding of this widely used substance and approach its use with greater caution.
The Synthetic Origins of a Medical Mainstay
Methylene blue was first synthesized in a laboratory in 1876 as a coal tar derivative. Its molecular structure, composed of heterocyclic rings containing sulfur and nitrogen, is entirely foreign to human biology. Unlike naturally occurring molecules that our bodies have evolved alongside, MB is a xenobiotic, meaning it is foreign to life processes.1
Despite its synthetic nature, methylene blue was rapidly adopted for medical use, starting with malaria treatment in the early 1900s.2 Over time, new applications were discovered—ranging from treating methemoglobinemia to acting as a urinary tract antiseptic, a surgical dye, and even as an experimental nootropic.3 However, its widespread adoption has occurred without long-term safety studies, making its continued use an ongoing human experiment.
The "Less is More" Paradigm: A Call for Caution
The conventional toxicology model assumes that below a certain threshold, substances cause no harm.4 However, modern research has shown that synthetic chemicals can exert biological effects even at infinitesimally small concentrations.
As I stated in my keynote presentation at Joel Salatin’s Polyface farms last summer:
"The 'dose makes the poison' is an outdated concept. We need a new model that recognizes the potential for harm even at extremely low doses."
If methylene blue can alter biological systems at such minuscule doses, we must ask: What are the long-term consequences of introducing this synthetic chemical into the body?5
Documented Adverse Effects: Raising Red Flags
While proponents of methylene blue tout its benefits, there is no shortage of documented adverse effects in the medical literature, albeit at doses higher than the biohacking community typically takes. Some of the most concerning include:
Serotonin Syndrome
Multiple case reports have described patients developing serotonin syndrome after receiving methylene blue, particularly when combined with serotonergic psychiatric medications. Serotonin syndrome is a potentially life-threatening condition caused by excessive serotonin activity in the nervous system.6
Hemolytic Anemia
Methylene blue has been associated with hemolytic anemia, particularly in patients with glucose-6-phosphate dehydrogenase (G6PD) deficiency. This potentially dangerous blood condition involves the premature destruction of red blood cells.7
Neurotoxicity
Multiple studies have documented neurotoxic effects of methylene blue, particularly at higher doses. A 2008 study in the journal Anesthesiology found that methylene blue had detrimental effects on the developing central nervous system in animal models.8
Cardiovascular Effects
Methylene blue can cause significant changes in blood pressure and heart rate. A review in the American Journal of Therapeutics noted:
"Methylene blue can cause severe hypertension when given in high doses, especially as an intravenous bolus. Other cardiovascular side effects include cardiac arrhythmias, coronary vasoconstriction, and decreased cardiac output."9
These documented effects are likely just the tip of the iceberg. Many adverse reactions may go unrecognized or unreported, especially more subtle long-term impacts. The full scope of methylene blue's effects on human health may not be apparent for decades.
Phycocyanin: A Natural Alternative to Methylene Blue
What is Phycocyanin?
Phycocyanin is a naturally occurring blue pigment-protein found in spirulina and cyanobacteria. It plays a vital role in photosynthesis and offers a powerful array of antioxidant, anti-inflammatory, and neuroprotective benefits—similar to those attributed to MB, but without the risks of synthetic interference associated with xenobiotic/petrochemically derived substances.
Spectral Overlap: Phycocyanin vs. Methylene Blue
Phycocyanin Absorption Peak: ~620-640 nm (overlapping with MB’s secondary peak at ~609 nm)
Phycocyanin Emission Peak: ~650-670 nm (close to MB’s primary peak at ~660-670 nm)
Shared Absorption Zone: ~610–650 nm—where both molecules are active.
This means that phycocyanin can serve the same purpose as MB in many therapeutic applications, including photodynamic therapy (PDT) and photobiomodulation, while avoiding MB’s synthetic toxicity.
Why Phycocyanin is Preferable to Methylene Blue
A Natural, Biocompatible Alternative
High Safety Profile
Millions of years of potential inclusion in the diet of the human species vs. only a few hundreds years for coal tar derivatives.
FDA-approved as a food colorant (E18 in the EU)
Oral LD50 (rats/mice): >5,000 mg/kg (suggesting very low toxicity)10
Comparatively, the Methylene Blue LD50: Oral ~1,180 mg/kg, IV ~44 mg/kg11
In other words, phycocyanin is over 4 times safer from the perspective of acute toxicity.
Conclusion: A Call for a Paradigm Shift
Methylene blue may have its place in emergency medicine, but its widespread use as a health supplement is problematic. The precautionary principle dictates that natural alternatives should be prioritized whenever possible.
Phycocyanin shares MB’s core benefits while avoiding its risks, making it a safer, natural alternative for those seeking enhanced mitochondrial function, cognitive support, and overall cellular health.
Here’s an example of an organic blue spirulina product high in phycocyanin that is affordable and easily available.
References
Caro, Heinrich. "Ueber die Einwirkung des Nitrobenzols auf aromatische Amine." Berichte der deutschen chemischen Gesellschaft 9, no. 1 (1876): 758–759. https://doi.org/10.1002/cber.187600901201.
Guttmann, Paul, and Paul Ehrlich. "Ueber die Wirkung des Methylenblau bei Malaria." Berliner Klinische Wochenschrift 28 (1891): 953–956. https://archive.org/details/berliner-klinische-wochenschrift-1891/page/953/mode/1up.
Quirk, Walter J. "Methylene Blue: An Old Drug with New Uses." Postgraduate Medicine 75, no. 4 (1984): 191–195. https://doi.org/10.1080/00325481.1984.11698730.
World Health Organization. WHO Model List of Essential Medicines: 22nd List, 2021. Geneva: World Health Organization, 2021. https://www.who.int/publications/i/item/WHO-MHP-HPS-EML-2021.02.
Ji, Sayer. "The Methylene Blue Paradox: When a Synthetic Dye Becomes a Health Trend." GreenMedInfo, October 17, 2024. https://greenmedinfo.com/blog/methylene-blue-paradox-when-synthetic-dye-becomes-health-trend.
Barras, Héritier, Pierre B. Maeder, and Jean-Michel Gaspoz. "Methylene Blue and Serotonin Syndrome: A Word of Caution." Journal of Neurology, Neurosurgery & Psychiatry 81, no. 2 (2010): 204. https://doi.org/10.1136/jnnp.2009.177329.
Liao, C. H., C. T. Lai, and C. C. Li. "Methylene Blue-Induced Hemolytic Anemia in a Patient with G6PD Deficiency: A Case Report." Veterinary and Human Toxicology 44, no. 1 (2002): 19–21. https://pubmed.ncbi.nlm.nih.gov/11824747/.
Vutskits, Laszlo, et al. "Adverse Effects of Methylene Blue on the Central Nervous System." Anesthesiology 108, no. 4 (2008): 684–692. https://doi.org/10.1097/ALN.0b013e318167af15.
Clifton, Jack, II, and Joel B. Leikin. "Methylene Blue." American Journal of Therapeutics 10, no. 4 (2003): 289–291. https://doi.org/10.1097/00045391-200307000-00010.
Romay, Chantal, et al. "C-Phycocyanin: A Biliprotein with Antioxidant, Anti-Inflammatory and Neuroprotective Effects." Current Protein & Peptide Science 4, no. 3 (2003): 207–216. https://doi.org/10.2174/1389203033487216.
National Center for Biotechnology Information. "Methylene Blue." PubChem Compound Summary for CID 6099. Accessed March 9, 2025. https://pubchem.ncbi.nlm.nih.gov/compound/Methylene-blue.
Sayer Ji's Substack
Welcome to my Substack—a space where I share insights, research, and reflections at the intersection of ancient wisdom and modern science. As the founder of GreenMedInfo.com, you will continue to receive health information to empower you here.
AND THIS:
Forwarded this email? Subscribe here for more
Synthetic Methylene Blues: When Biohackers Choose Petroleum Over Plants
The cognitive dissonance of rejecting food dyes while swallowing industrial chemicals — and the natural pigments that make methylene blue obsolete
AUG 23
Following up on "The Blue Brain Effect: Methylene Blue's Dark Side & What You Should Be Using Instead," this deep dive explores the full scope of methylene blue's underreported toxicity and presents nature's superior alternatives for photobiomodulation and cognitive enhancement.
Read, share, and comment on the X thread dedicated to this article here: https://x.com/sayerjigmi/status/1958377526453027055
It sounds like something out of a Victorian dye factory: a coal tar-derived petroleum dye from the 19th century being ingested by modern health enthusiasts. Yet that is precisely the paradox of methylene blue (MB). Discovered in 1876 by German chemists for coloring textiles¹, MB is an aniline-derived synthetic (i.e. a brown, oily petroleum-derived product)that today finds itself touted as a ‘nootropic’ and ‘mitochondrial booster’ in certain biohacker circles.
Wellness influencers have promoted its electric-blue drops for enhanced cognition and cellular energy. But behind the trendy blue tongue photos lies an unsettling truth: if we'd reject coal tar dyes in our food or skincare, why would we welcome them into our brain?
Picture a health-conscious individual swirling a vial of brilliant blue solutionand downing it for "brain fuel." The liquid's vivid hue comes from the same industrial dye class once used to stain cloth. Methylene blue owes its lineage to petrochemical coal-tar chemistry, a far cry from the natural herbal tonics one might expect of holistic health. The irony is rich: a community that rightfully shuns artificial food coloring is embracing a synthetic dye as a supplement.
How did we get here? Proponents argue MB can enhance mitochondrial function and even act as a neuroprotective agent. But emerging evidence paints a far less rosy picture.
Methylene Blue: From Antidote to "Nootropic" Fad
Methylene blue has a long history in medicine, primarily as an emergency antidote and diagnostic tool. In clinical settings, MB is used to treat methemoglobinemia (a life-threatening inability of blood to carry oxygen), to manage ifosfamide-induced neurotoxicity, as a last-resort therapy in vasoplegic shock, and as a surgical dye for imaging². These uses leverage MB's pharmacological actions — it can accept and donate electrons in cells, inhibit nitric oxide (NO) signaling (raising blood pressure), and assist in restoring hemoglobin function².
In other words, MB is deployed as a "lesser evil" in acute crises, where its benefits may outweigh risks for a short period. It was never designed to be a daily cognitive enhancer.
Despite this, a trend has emerged: some biohackers now take microdoses of MB regularly, hoping to boost brain energy metabolism. This off-label use was spurred by early studies suggesting MB might support mitochondrial respiration or memory under certain conditions. However, translating a chemical antidote into a wellness supplement is a dubious leap.
MB received an FDA black-box warning in 2011 due to dangerous interactions with common antidepressants; it can trigger potentially fatal serotonin syndrome when combined with SSRIs³. Far from being a harmless vitamin, MB is a potent monoamine oxidase inhibitor at higher doses³ — effectively a drug that modulates brain chemistry. Before anyone adds this blue dye to their smoothie, it's crucial to examine the science of its safety.
The Dark Side of Methylene Blue: What Science Reveals
Enthusiasts claim methylene blue "powers up" mitochondria and neurons. But peer-reviewed research and case reports reveal serious liabilities:
Neurotoxicity and Electrophysiological Disruption
In vitro studies have shown that MB can damage neurons and impair their electrical function at surprisingly low concentrations. Mouse sensory neurons exposed to MB in the micromolar range suffered dose-dependent toxicity — by 10 µM, many neurons lost their neurites (branches) and degenerated⁴.
What does this 10 µM threshold actually mean for your brain?
To understand the implications, let's break down the numbers. A concentration of 10 µM (micromolar) equals approximately 3.2 micrograms per milliliter of fluid — or about 0.003 milligrams per milliliter. At this seemingly minuscule concentration, neurons in laboratory studies begin to malfunction dramatically. They lose their ability to communicate properly with other cells, their branches (dendrites and axons) wither away, and eventually the cells die altogether⁴.
This is particularly concerning when you consider that many methylene blue supplements recommend doses of 0.5–4 mg. While we can't directly equate a supplement dose to brain tissue concentration (due to variables like absorption rates, blood-brain barrier penetration, and individual metabolism), the forensic evidence of blue-green brain staining at autopsy proves that MB does accumulate in neural tissue⁵.
Think of it this way: if your morning coffee started killing brain cells after just a few sips rather than requiring massive overdose, you'd reconsider that daily cup. Yet that's essentially what these studies reveal about methylene blue — the margin between its promoted "nootropic" dose and documented neurotoxic effects is alarmingly narrow.
Electrophysiological recordings from nerve cells treated with MB revealed even more troubling effects. The neurons showed diminished electrical currents and blunted action potentials⁴. In essence, MB makes it harder for neurons to fire properly, slowing their signals and reducing their ability to generate the electrical impulses that underlie all brain function. These findings align with earlier reports in brain tissues and gut neurons showing that MB exposure leads to neuronal loss and altered membrane properties⁴.
The take-home point: the same chemical that might prop up a failing mitochondrion in emergency medicine can, at concentrations easily achievable through supplementation, poison the neuron itself. What's marketed as "brain fuel" operates on a razor's edge between enhancement and harm — and the science suggests we're playing with fire when we treat this industrial dye as a daily vitamin.
Bioaccumulation in Brain and Organs
One of the most striking (and unsettling) illustrations of MB's impact comes from forensic medicine. Pathologists performing autopsies on patients who received MB have noted a bizarre phenomenon: the brain (and sometimes heart) emerges stained an eerie blue-green color⁵.
Image source: Durão, C., Pedrosa, F. & Dinis-Oliveira, R.J. Greenish-blue discoloration of the brain and heart after treatment with methylene blue. Forensic Sci Med Pathol 17, 148–151 (2021). https://doi.org/10.1007/s12024-020-00316
A 2024 study titled "Fifty shades of green and blue: autopsy findings after administration of xenobiotics" reported that systemic methylene blue use before death led to dark blue-green discoloration of organs, especially the brain⁵. In multiple cases, patients treated with MB for shock or poisoning were found on autopsy to have vivid blue-green brains⁵.
This occurs because MB (a lipophilic cation) readily penetrates the brain and gets reduced to a colorless form in vivo — but upon exposure to air post-mortem, it oxidizes back to blue, revealing its presence dramatically⁵,⁶. The images (published by forensic teams) are jarring: a human brain with turquoise-blue hues infiltrating the tissue.
As one Substack commenter quipped, "If this is what methylene blue in the brain post-mortem looks like, what is it doing while you're alive?" In living patients, that dye is presumably lodging in neurons and glia. MB's half-life is ~5-6 hours in plasma⁸, but its affinity for certain tissues means residues can linger — indeed, it is known to tint the urine blue or green as it slowly clears⁵. The autopsy data prove that MB crosses the blood-brain barrier and accumulates, which should give any neurohacker pause.
Suppressed Brain Blood Flow and Metabolism
Paradoxically, the very outcome biohackers desire — enhanced brain energy and perfusion — may be undermined by MB in healthy individuals. A placebo-controlled study published in 2023 examined acute MB administration in humans using advanced neuroimaging⁷.
The researchers expected MB to boost cerebral oxygen consumption (based on test-tube studies of mitochondrial enzymes), but instead found the opposite. MB reduced global cerebral blood flow (CBF) in healthy volunteers by a significant degree, at doses of 0.5–1 mg/kg i.v.⁷ It also decreased the brain's metabolic rate of oxygen (CMRO₂) — meaning the brain was using less oxygen — compared to baseline⁷. In parallel experiments, rats given MB showed a drop in cerebral glucose metabolism⁷.
These effects were dose-dependent and consistent across species. The authors concluded that MB at clinically relevant doses can exert an inhibitory effect on brain energy metabolism in normal brains⁷. The likely mechanism is related to MB's strong inhibition of nitric oxide signaling². By scavenging NO and blocking guanylate cyclase, MB causes blood vessels to constrict². Less blood flow means less oxygen and glucose delivered to brain tissue.
In a diseased brain with mitochondrial dysfunction, a small MB dose might act as an electron shuttle and improve efficiency (a hormetic effect). But in a healthy brain, those same doses appear to overshoot into a metabolic suppression. So while anecdotes claim mental clarity on MB, the hard data show that in healthy humans MB can decrease cerebral perfusion and metabolism⁷ — hardly a biohacking win.
Serotonin Syndrome and Neurochemical Chaos
MB's biochemical actions are wide-ranging, and that breadth comes with risks. At higher systemic doses, MB and its metabolites inhibit monoamine oxidase (particularly MAO-A)³,⁴. This means MB can amplify serotonin levels in the brain — dangerously so if combined with other serotonergic agents.
The FDA's black-box warning on MB is there for good reason: cases of serotonin syndrome (a life-threatening toxic state) have occurred when MB was given to patients on antidepressants³. Symptoms can include high fever, muscle rigidity, agitation, and seizures — a medical emergency. For example, in one published case, a cancer patient treated with MB for ifosfamide-induced encephalopathy developed severe serotonin syndrome and had to be admitted to intensive care³.
MB was the trigger that, combined with an SSRI in the patient's regimen, sent serotonin signaling into overdrive. Several deaths have been reported after the combination of an MAOI (like MB in this context) with an SSRI². Even on its own, MB's serotonergic toxicity can manifest as confusion, neuromuscular hyperactivity (tremors, clonus), and autonomic instability².
This is not a gentle compound — it acts on neurotransmitter systems in ways that are not fully predictable, especially outside a controlled medical setting. For anyone self-medicating with MB, the message is clear: you are tinkering with a drug that can push the brain's serotonin network into chaos if misused.
Pro-oxidant and Cytotoxic Effects
While often billed as an "antioxidant" or mitochondrial protectant, MB can alsopromote oxidative stress under certain conditions. Research shows that MB increases production of superoxide (a reactive oxygen species) when it inhibits NO signaling². The result can be heightened inflammatory activity and cellular damage.
In ischemic tissues, for example, MB has been noted to exacerbate injury at high doses by impairing microcirculation⁶. An animal study found that large doses of MB during endotoxemia actually worsened hypotension and heart function, whereas low doses had the opposite effect⁶. This highlights MB's narrow therapeutic window.
On a cellular level, MB exposure has been linked to apoptosis and necrosis of tissue. Cases exist of local tissue death: for instance, a mere 1% MB injection (intravenous) causing skin necrosis at the site², or mucosal ulceration from submucosal MB use². These are extreme outcomes, but they underscore that MB is fundamentally a toxin — it kills microbes (and can kill cells) by generating oxidative stress.
Even its beneficial actions (like treating methemoglobinemia) rely on its pro-oxidant chemistry to some extent, as it cycles between oxidized and reduced forms. Thus, using MB chronically might expose the body to continuous low-grade oxidative stress. Indeed, countries such as Canada have classified MB as harmful for general consumer use due to risks like skin irritation and inflammatory reactions².
A "Last Resort" Drug, Not a Daily Tonic
Perhaps the most salient point is context. MB's role in medicine is as an antidote or diagnostic stain — essentially, a tool to be used sparingly when needed. It is not approved as a daily prophylactic supplement.
As a 2022 toxicology review bluntly stated, the basic toxicological characteristics of MB remain inadequately studied, and its clinical use is "controversial" given reports of severe adverse effects that *"could significantly exceed any possible benefits"². In other words, even in critical care where MB might be indicated, doctors must weigh its toxicity heavily.
There are no long-term studies on healthy people taking methylene blue regularly. What we do know comes from short-term emergency use and lab studies — and much of that knowledge waves red flags. MB can cause hemolytic anemia in people with G6PD enzyme deficiency, for example, and can spike blood pressure or precipitate arrhythmias.
The precautionary principle would dictate that we don't blithely experiment on ourselves with such a compound, certainly not when safer alternatives exist. As the toxicology review concluded, the clinical use of MB without robust safety data "conflicts with the standards of safe use" in medicine². All this underscores a key ethical point for the natural health community: If we chastise pharmaceutical drugs for their side effects and demand rigorous safety evidence, should we not hold methylene blue to the same standard?
Nature's Photodynamic Alternatives: Pigments That Heal
One reason methylene blue attracted biohackers is its unusual property as a photodynamic compound: it absorbs light in the red/near-infrared range (~600–700 nm) and can influence mitochondrial processes. But MB is not unique in this regard. Many natural pigments — the very ones that color the plants and foods in a healthy diet — have similar light-absorbing characteristics and often superior safety profiles.
Chlorophyll & Chlorophyllin (Green Plant Pigments)
Chlorophyll is the life-blood of plants, the green pigment that captures sunlight for photosynthesis. It just so happens that chlorophyll's absorption spectrum overlaps significantly with methylene blue's. Chlorophyll a has a strong absorption band in the red (~660 nm) and another in the blue (~430 nm).
Chlorophyll mainly grabs red and blue light, while letting green light through — nearly the inverse of melanin's broad absorbance¹⁵. This means when you consume chlorophyll (e.g., as fresh wheatgrass or spinach, or as a chlorophyllin supplement), you are introducing a molecule that can absorb red/NIR light inside your body.
Researchers have begun to leverage chlorophyll derivatives in photodynamic therapy (PDT) for cancer, precisely because of this property. Sodium copper chlorophyllin, a water-soluble form of chlorophyll, has an intense absorption peak around 630 nm¹², ideal for red-light activation. In PDT studies, modified chlorophyllin compounds were able to localize to mitochondria and, under red light, produce singlet oxygen to kill tumor cells — in fact, some chlorophyllin-based photosensitizers outperformed methylene blue in efficacy¹².
The key point for our purposes is that chlorophyllin is remarkably safe (it's even used as a food colorant and deodorizer)¹², and it can interact with light in the same therapeutic window (600–700 nm) that MB does.
Beyond photodynamics, chlorophyll offers intrinsic health benefits. It's a potent antioxidant and metal chelator, known to bind and help eliminate certain toxins. Some visionary biochemists suggest that consuming chlorophyll-rich foods may aid human energy production. For instance, a 2014 study by researchers at Washington University proposed that a chlorophyll metabolite can integrate into mammalian mitochondria and enhance ATP production when exposed to light¹³.
Phycocyanin (Blue Spirulina Pigment)
If you've seen the surge of turquoise smoothies and lattes on Instagram, you might know "blue spirulina." The vivid aqua-blue color comes from phycocyanin, a brilliant blue pigment-protein complex found in spirulina and other cyanobacteria.
Phycocyanin is essentially the photosynthetic pigment that complements chlorophyll in those organisms — it absorbs light in the orange/red part of the spectrum and transfers energy to chlorophyll for photosynthesis. Remarkably, phycocyanin's spectral profile overlaps with methylene blue's almost hand-in-glove. It has a major absorption peak around 620–640 nm, which coincides with MB's secondary peak (~609 nm), and it emits fluorescence around 650–670 nm, near MB's primary peak (~664 nm)¹⁴.
In practical terms, phycocyanin can absorb and respond to 600–670 nm light just like MB does¹⁴. This makes it a natural candidate for photodynamic and photobiomodulation therapies. Indeed, researchers have noted that phycocyanin can serve the same purpose as MB in many light-based applications (like PDT), without MB's synthetic toxicity¹⁴.
Importantly, phycocyanin is highly biocompatible and safe. It's a protein you're essentially eating whenever you consume spirulina or blue-green algae supplements. A 2003 review by Romay et al. documented phycocyanin's impressive antioxidant, anti-inflammatory, and neuroprotective effects⁹. It scavenges free radicals and inhibits COX-2, tempering inflammation. In models of neurodegenerative disease and stroke, phycocyanin has shown protective outcomes, presumably by quenching oxidative stress and modulating immune responses⁹.
Notably, phycocyanin crosses the blood-brain barrier and can support brain health without staining your brain blue. In my previous analysis of MB below, I highlighted that phycocyanin appears to be over four times safer than MB in terms of acute toxicity¹⁴. There's no known "phycocyanin syndrome," no MAOI interaction issues, and no reports of it turning people's organs strange colors.
The Blue Brain Effect: Methylene Blue’s Dark Side & What You Should Be Using Instead
MAR 9
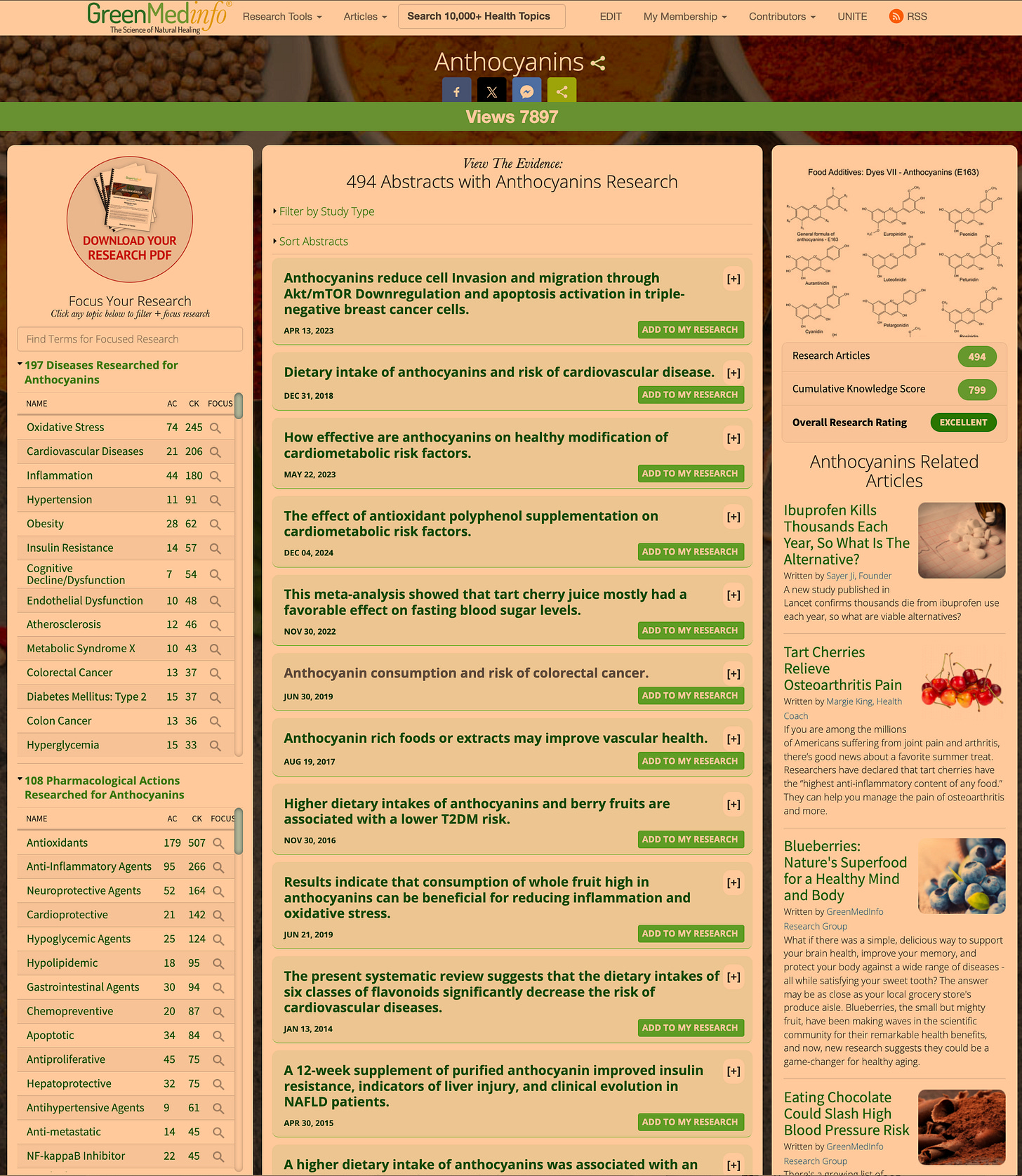
Anthocyanins (Purple-Blue Plant Antioxidants)
Anthocyanins are the pigments that give berries, purple carrots, red cabbage, and butterfly pea flowers their rich red-blue-violet hues. Structurally flavonoids, anthocyanins are powerful antioxidants and anti-inflammatories, and they have a special affinity for the brain.
Numerous studies show that anthocyanin-rich foods improve cognitive function and protect neurons¹⁰. They combat neuroinflammation and oxidative stress — two key drivers of brain aging and neurodegenerative diseases. In fact, diets high in blueberries and other anthocyanin sources are linked to a reduced risk of dementia and better memory in older adults¹⁰. In fact, on GreenMedInfo.com, we have indexed research on its broad spectrum therapeutic potential across almost 200 different conditions.
Unlike methylene blue, which might cause oxidative stress, anthocyanins vigorously oppose it, quenching free radicals and chelating metal ions that catalyze oxidative damage¹⁰. This makes them inherently neuroprotective.
From a photonic perspective, anthocyanins absorb light in the visible range, particularly in the green-yellow spectrum, and depending on pH can extend into the orange-red. For instance, the blue butterfly pea flower (Clitoria ternatea) yields an anthocyanin-rich extract that at neutral pH is deep blue. Spectral analysis of butterfly pea extract shows absorption peaks around 572 nm and 614 nm¹¹, squarely within the visible range and encroaching on the red/NIR boundary.
A practical way to harness anthocyanins is through diet and herbal teas. Butterfly pea flower tea has gained popularity as a caffeine-free cognitive tonic — it brews into a striking blue potion, which can turn purple with a squeeze of lemon (changing pH). This tea provides a natural anthocyanin dose that some compare to a "nature's blue tonic."
Melanin (The Broad-Spectrum "Solar Panel" Pigment)
Melanin is perhaps the most underappreciated bio-pigment when it comes to human health. We usually think of melanin only as a skin pigment for UV protection or the coloring of hair and eyes. But melanin is everywhere in nature — from fungi and bacteria to the ink of cephalopods — and it has astonishing biophysical properties.
Melanin can absorb a broad swath of the electromagnetic spectrum, from ultraviolet through visible light and well into the infrared¹⁵. In other words, it's a "universal absorber," earning nicknames like "the biological black hole." Unlike chlorophyll (which has defined peaks) or MB (which mainly absorbs around 660 nm), melanin shows a continuous absorption that increases toward the UV but still extends into IR wavelengths¹⁵.
In the context of photobiomodulation, this is huge. Red and near-infrared light (600–850 nm) are widely used to heal tissues and energize mitochondria — a field known as photobiomodulation (PBM)¹⁵. Melanin, being a broad-spectrum absorber, can soak up these PBM wavelengths and potentially transduce them into useful forms of energy or signaling in the body.
Emerging research suggests melanin might act as a sort of biophotonic engine: it can convert absorbed photons into other energy, possibly by splitting and reforming water molecules at the microscopic level¹⁵. Experiments have shown that exposing melanin to light does boost electron transfer reactions and can even lead to the production of electrical energy or chemical energy¹⁵.
The Ultimate Human Superpower You Never Knew You Had: Melanin — The Hidden Solar Panel in Human Biology
·
JUL 24
How does this relate to brain health? Intriguingly, our brains naturally contain a form of melanin — neuromelanin — concentrated in regions like the substantia nigra and locus coeruleus (which appear dark due to it). The fact that key brain nuclei are loaded with neuromelanin (giving them that dark hue) hints at a purpose¹⁵. Those cells are involved in movement, mood, and wakefulness, and they also happen to be the ones that die off in Parkinson's disease (PD), where neuromelanin is lost.
What we do know is melanin is biocompatible (it's part of us) and can be supplemented to some extent through diet. Certain foods and herbs contain melanins or melanin precursors: for example, black sesame seeds, black rice, cacao, coffee, and some mushrooms have high melanin or polyphenols that stimulate melanin pathways.
Rethinking the "Lesser Evil" Philosophy in Medicine
The rise of methylene blue as a supplement reflects a broader issue in both conventional and alternative medicine: the tendency to treat symptoms or downstream effects while tolerating (or ignoring) upstream causes. In hospital medicine, MB is often used as a "Hail Mary" antidote, a lesser evil to counteract a greater evil.
What's troubling is when this model migrates into daily health practice, especially in the holistic community that normally advocates addressing root causes. If someone feels fatigue or brain fog (common issues), reaching for a petrochemical derivative like methylene blue might perk them up by forcing certain pathways — but it could also be masking an underlying issue like poor mitochondrial function, heavy metal toxicity, chronic inflammation, or nutrient deficiencies. Rather than investigate and resolve those root causes, one might be displacing the problem with a quick chemical or pharmacological fix.
Moreover, embracing MB sends a mixed message in natural health advocacy. On one hand, we campaign to ban coal-tar food dyes (like Blue #1, a cousin of MB) because of their neurotoxicity and potential to cause ADHD in kids. We avoid artificial colors in supplements and demand whole-food sources of nutrients. And yet, MB — literally a coal-tar derived aniline dye⁴ — gets a pass because it's been rebranded as a nootropic?
If we oppose petrochemical dyes in our food, we must apply the same skepticism to petrochemical dyes in our brain. The chemical doesn't get sanctified just because someone on a podcast calls it "mitochondrial medicine." We should recall that MB was first synthesized to kill life (textile dyes often doubled as antiseptics and antiparasitics). Its widespread use preceded the era of rigorous drug safety testing — in fact, a 2022 review lamented that MB has been used for 140+ years "without a clearly defined pharmacotoxicological frame of reference," and that fundamental toxicity data are missing².
Building a Brain-Boosting Photobiological Stack (Sans Methylene Blue)
So, what might a practical, natural "photobiology stack" look like for someone seeking the benefits that methylene blue promises? Here's a blueprint that combines the pigments and principles we've covered:
Start with a Pigment-Rich Breakfast: Instead of a blue dye drop, begin your day with a blue-green smoothie or elixir. For example, blend organic spirulina (for phycocyanin and chlorophyll) into a smoothie with wild blueberries or blackberries (for anthocyanins). Add a handful of spinach or moringa powder (for extra chlorophyll and magnesium).
Red Light Exposure: After fueling up on those pigments, spend some time in morning sunlight or under a red/near-infrared light therapy device. Sunlight in the early morning has a good amount of near-infrared, which penetrates deeply. These wavelengths will interact with the pigments now circulating in your bloodstream.
Cofactors and Neuroprotective Nutrients: Alongside pigments, consider key mitochondrial cofactors and neuroregenerative supplements:
Coenzyme Q10 (ubiquinol is the ‘reduced’ and fully bioactive form) and PQQ: Support the electron transport chain and mitochondrial biogenesis
B-Vitamins (B2, B3, B12) and Magnesium: Direct precursors for FAD and NAD
Lion's Mane Mushroom & Bacopa Monnieri: Famed neuroregenerative herbs
Omega-3 Fatty Acids (DHA): Essential for brain membrane health
Melatonin (at Night): A mitochondrial antioxidant and repair signal
Healthy Habits in Tandem: No stack is complete without the basics. Regular physical activity, good sleep hygiene, and a clean diet low in processed toxins will amplify all the above.
This kind of protocol — call it a "photonic nutrition and PBM stack" — epitomizes a holistic biohack. You are nourishing the body with natural compounds that it can incorporate into cells, and then activating them (and your innate chromophores like cytochrome and melanin) with therapeutic light.
Conclusion: Choosing Coherence and Caution in Our "Blue" Choices
In the journey of natural health, coherence is key. We strive to align our interventions with the body's design and with principles that hold true across domains. If we condemn artificial dyes in our food for being neurotoxic or disruptive, we must hold methylene blue to the same scrutiny.
The emerging field of biophotonic medicine is incredibly exciting. It teaches us that light and pigments are as much a part of nutrition and healing as vitamins and herbs. We are, in a sense, "light eaters" and "light emitters." Methylene blue was an eye-opening part of that discovery process — it demonstrated that a chemical could modulate biochemistry through photochemical means. But it's not the end of the story, nor the pinnacle of it.
Rather, it's a stepping stone pointing back to what biology has used all along: chlorophyll to capture sunlight and fuel life, melanin to absorb the full spectrum and protect (or possibly energize) tissues, anthocyanins to guard plants (and brains) from oxidative stress, phycocyanins to bridge the gap between sunlight and biochemical energy. These are time-tested, harmonious agents that our bodies know how to handle.
By adopting strategies that include these natural pigments and sensible light exposure, we honor a core holistic tenet: support the body's innate healing and adaptive systems, don't supplant them.
If coal-tar dyes have no place in our food or on our skin, they certainly have no place being touted as daily brain enhancers. We have cleaner, greener (and bluer and blacker!) options at our fingertips. By choosing those, we stand for coherence in natural health advocacy.
References
Caro, Heinrich. "Über die Einwirkung des Nitrobenzols auf aromatische Amine." Berichte der deutschen chemischen Gesellschaft 9, no. 1 (1876): 75–759.
Buzgă, Marek, et al. "Methylene blue: a controversial diagnostic aid and medication?" Toxicology Research 11, no. 5 (2022): 711–717.
Snyder, Matthew, et al. "Serotonin syndrome complicating treatment of ifosfamide neurotoxicity with methylene blue." Cancer Control 24, no. 5 (2017): 1–4.
Horrmann, Alec, et al. "Adverse effects of methylene blue in peripheral neurons: An in vitro electrophysiology and cell culture study." Molecular Pain 18 (2022): 17448069221142523.
Baumgarten, J., I. Greb, et al. "Fifty shades of green and blue: autopsy findings after administration of xenobiotics." Forensic Science, Medicine, and Pathology (2024, online ahead of print).
Durão, Carlos, et al. "Greenish-blue discoloration of the brain and heart after treatment with methylene blue." Forensic Science, Medicine, and Pathology 17, no. 1 (2021): 148–151.
Singh, Nisha, et al. "The effects of acute methylene blue administration on cerebral blood flow and metabolism in humans and rats." Journal of Cerebral Blood Flow & Metabolism 43, suppl. 2 (2023): 95–105.
Heyman, Peter, and Robert Klotz. "Pharmacokinetics of methylene blue in man." Clinical Pharmacology & Therapeutics 25, no. 3 (1979): 332–338.
Romay, Chantal, et al. "C-Phycocyanin: A biliprotein with antioxidant, anti-inflammatory and neuroprotective effects." Current Protein & Peptide Science 4, no. 3 (2003): 207–216.
Henriques, Joana F., et al. "The anti-neuroinflammatory role of anthocyanins and their metabolites for the prevention and treatment of brain disorders." International Journal of Molecular Sciences 21, no. 22 (2020): 8653.
Saptarini, Nyi M., et al. "Application of Butterfly Pea (Clitoria ternatea L.) extract as an indicator of acid-base titration." Journal of Chemical and Pharmaceutical Research 7, no. 2 (2015): 275–280.
Uchoa, Adjaci F., et al. "Chlorophyllin derivatives as photosensitizers: Synthesis and photodynamic properties." Journal of the Brazilian Chemical Society 26, no. 12 (2015): 2571–2585.
Pollack, Gerald H., et al. "Molecules, water, and radiant energy: New vistas for cytochemistry." Acta Histochemica et Cytochemica 47, no. 1 (2014): 1–8.
Ji, Sayer. "The Blue Brain Effect: Methylene Blue's Dark Side & What You Should Be Using Instead." Substack, March 9, 2025.
Ji, Sayer. "The Ultimate Human Superpower You Never Knew You Had: Melanin — The Hidden Solar Panel in Human Biology." Substack, 2025.
AND THIS ARTICLE FROM Dr Peter Breggin
Breggin Alerts! Exposing Global Predators
Emergency notification: methylene blue is highly neurotoxic to your brain and mind
methylene blue is a Monoamine Oxidase Inhibitor (MAOI). As such, it is one of the most toxic agents ever used in medicine and psychiatry, and the mother of the most dangerous drugs used in psychiatry
May 18, 2025
In reality, methylene blue is a lethal neurotoxin, a poison to the brain. It has the same basic chemical composition and harmful clinical effects as the oldest and most neurotoxic “antidepressants,” the monoamine oxidase inhibitors (MAOIs). It also has similarities to the neurotoxic phenothiazine “antipsychotic” drugs, including the original Thorazine (chlorpromazine), but methylene blue is more stimulating or activating.
Methylene blue is not a miraculous new discovery. It’s the opposite. Created in 1876 in a lab, it is the oldest manmade chemical to be used in medicine. But for well over a century, methylene blue has never been FDA-approved for psychiatric purposes. Later, its chemical structure was modified in labs to create many of the earliest, most neurotoxic psychiatric drugs.
Methylene blue is widely marketed over the counter to the general public as well as to the natural health, health freedom, and freedom communities, often on the internet. It’s flooding America.
Some sellers are touting methylene blue as a “miracle” tonic that improves “cognitive function”1 and boosts energy to previously unimagined heights. Some have given live demonstrations on TV and podcasts demonstrating how the oral form hyperactivates some people within 35 minutes of the first dose — a typical stimulant drug rush—which is actually a danger signal for potentially activating them into a dangerous manic episode during future exposures or even more deadly outcomes.
Methylene blue suppresses or destroys forms of the enzyme monoamine oxidase that are used by the brain for controlling or modulating four different powerful neurotransmitters — serotonin, dopamine, norepinephrine, and epinephrine. In short, by crushing monoamine oxidase, methylene blue causes overstimulation of four of the brain’s major neurotransmitters, all of which profoundly impact the mind.
After the FDA was created in 1906, methylene blue was grandfathered into the market by the agency as an obscure antidote for methemoglobinemia, but it must be emphasized that the FDA has never tested the safety of methylene blue for any purpose. Furthermore, the FDA, based on its adverse reporting system and scientific reports, has published serious warnings about potentially lethal adverse reactions from methylene blue, especially when combined with numerous other drugs.2
The first MAOIs used as depressants were derived from methylene blue, and they turned out to be so toxic that the first two were quickly taken off the market by the FDA. One caused lethal liver disease, and the other caused hypertensive crises. Methylene blue is known to impair liver function tests and to cause hypertensive crises. Early on, all MAOIs were removed for a while from the international list of approved drugs. Please go to this endnote in my report for a list of historical and scientific studies about the extraordinary history and the nature of methylene blue and the other MAOIs.3
Psychiatry and the psychopharmaceutical complex are so driven to impose neurotoxins upon our brains that some MAOI antidepressants remain on the market today. FDA Full Prescribing Information for the existing MAOI antidepressants, readily available online,4 provides quick access to the kinds of adverse effects caused by methylene blue. These FDA documents also provide lists of the foods and of some of the many, many drugs you cannot take with MAOIs, like methylene blue, without risking death from serotonin syndrome or a hypertensive crisis.
Meanwhile, all of America is being made a market for the original mother of them all, methylene blue, without requiring a prescription, with bizarrely distorted claims, and with unlimited supplies handed out as easily as a new caffeinated soda.
All of the three approved MAOIs, as well as methylene blue, carry repeated warnings at the FDA and in the scientific community about causing the two potentially crippling and lethal outcomes, serotonin syndrome and malignant hypertension (see below). These potentially lethal outcomes, as with all MAOIs, become much more serious and higher risk when methylene blue is taken with certain foods such as cheese and bananas, or literally with so many other drugs that it is impossible to memorize them or to keep track of them.
Here is one version of a short summary of the long list of dangerous interactions between MAOIs, including methylene blue, and other drugs and foods, taken from Goodman and Gilman’s The Pharmacological Basis of Therapeutics (2018, p. 274):
Monoamine Oxidase Inhibitors
Serotonin syndrome is the most serious drug interaction for the MAOIs (see Adverse Effects). The most common cause of serotonin syndrome in patients taking MAOIs is the accidental co-administration of a SHT reuptake-inhibiting antidepressant or tryptophan. Other serious drug interactions include those with meperidine and tramadol. MAOIs also interact with sympathomimetics such as pseudoephedrine, phenylephrine, oxymetazoline, phenylpropanolamine, and amphetamine; these are commonly found in cold and allergy medication and diet aids and should be avoided by patients taking MAOIs. Likewise, patients on MAOIs must avoid foods containing high levels of tyramine: soy products, dried meats and sausages, dried fruits, home-brewed and tap beers, red wine, pickled or fermented foods, and aged cheeses.
I am presenting this detailed summary in the hope of gaining the immediate attention of people and businesses who are promoting methylene blue and anyone who is unfortunately taking it. Please share this summary or the entire document as widely as possible and with proper attribution.
This article continues with my professional experience in psychopharmacology, followed by a lengthy scientific analysis with more than two dozen endnotes containing an even greater number of scientific citations.
Podcast: Play in new window | Download | Embed
Listen to the podcast on this story here: Emergency notification for methylene blue! It’s highly neurotoxic to your brain and mind
Editor’s note: This column is too long for email—to read the entire column please click on the headline above or click here to go to the Breggins’ Substack and this complete column.
My Background in Psychopharmacology Related to Analyzing Methylene Blue
In presenting this emergency notice on the dangers of methylene blue, I am drawing on a lifetime of professional work, starting with my own published animal laboratory research while a medical student.5 My research demonstrated for the first time that exposures of animals to intramuscular adrenaline (a combination of epinephrine and norepinephrine) might give initial activation or stimulation, but that more prolonged exposure over a few minutes or hours made the animals sedated, exhausted, sluggish, or blunted for the duration of their drug exposure. I hypothesized that a feedback mechanism to the hypothalamus caused a compensatory reaction that slowed down the brain and made the animals sluggish.
Methylene blue is in the biochemical and clinical classification of Monoamine Oxidase Inhibitors (MAOIs) used as “antidepressants,” but it has no FDA testing for safety! It has all the same hazards as the FDA-approved MAOIs for depression and is probably biochemically more harmful or neurotoxic. It is made even more dangerous in the manner in which it is sold, marketed without medical supervision as a powder or liquid, with unlimited doses made available at once, and with enormously unrealistic expectations and no extensive warnings.
Since becoming a psychiatrist, I have written many scientific papers and many books6 showing how human beings who take psychiatric drugs sometimes are initially stimulated when the drug over-activates the monoamine neurotransmitters, including epinephrine, norepinephrine, serotonin, and dopamine; but eventually, similar to the animals, the human drug recipients typically become more subdued, apathetic, or disengaged from their own feelings, those around them, and with life itself.
Since the 1970s, I have researched, published, lectured, consulted, and testified in court about adverse drug effects. I have been a medical consultant and expert in hundreds of malpractice, negligence, and product liability lawsuits against drug companies, medical facilities, and medical doctors who make, market, or prescribe these neurotoxins, including consultations to the FAA (about pilots taking antidepressants), to a committee of U.S. attorneys general, and to several committees of the U.S. Congress.7 I have also testified in court more than 100 times, mostly about adverse drug effects causing very serious outcomes such as psychosis, mania, violence, and suicide.
Because they do more harm than good, I do not prescribe psychiatric drugs as a treatment in my clinical practice. Instead, I offer individual and family therapy, as well as education on more effective and healthier principles of living. However, I have specialized for decades in withdrawing patients from the medications given to them by other prescribers, which continues to provide me with considerable personal experience with prescribing these medications.
I am the author of the only medical textbook on the subject, called Psychiatric Drug Withdrawal: A Guide for Prescribers, Therapists, Patients and Their Families.
Destructive Claims for Methylene Blue
Within the general population as well as the freedom and health freedom communities, methylene blue is now being heralded as a nearly harmless potion that will improve all of our lives, backed online by testimonials of well-known freedom fighters and researchers. One demonstration shows that in 30 minutes, we will feel better than ever, lifting our usual physical and mental functioning to new levels. Some of the individuals look and sound very “hyper” and even mildly euphoric, with some distortions in perception and thinking. That means that the individual has taken a truly toxic drug and is in more grave danger with continued use.
In particular, methylene blue is credited with “cognitive enhancement” and who among us wouldn’t like more of that — especially when we’re so stressed or overworked? Methylene blue is being marketed by businesses and people within the health freedom and freedom movements as a “miracle” and a “silver bullet” for everything you can imagine.
I will not at this time name any person or any business who is promoting methylene blue, some of whom I know and even love. My hope is that they will hear the truth and simply stop marketing it, and hopefully stop taking it themselves. Ultimately, the widespread use of methylene blue, especially among freedom-oriented people and some of their most revered leaders, is one more threat to the survival of human freedom.
Overview of the Impact of Neurotoxins on the Lives of Humans
Most people taking psychiatric drugs eventually lose the intensity of caring required to defend freedom. All psychoactive drugs, and MAOI “antidepressants,” are especially neurotoxic, eventually robbing individuals of their own personal sovereignty and their motivation and ability to defend their rights. And as we shall demonstrate, these same drugs rob individuals of their ability to understand how badly impaired they have become by the drugs. I call it medication spellbinding (see below).
Methylene Blue is a Highly Toxic Monoamine “Antidepressant”
As already emphasized, methylene blue is a Monoamine Oxidase Inhibitor (MAOI). As such, it is one of the most toxic agents ever used in medicine and psychiatry, and the mother of the most dangerous drugs used in psychiatry today.
Their severe adverse effects can be confirmed by looking at the FDA’s Full Prescribing Information or Label for any of the other MAOI antidepressants. Although most psychiatrists know enough to avoid prescribing them, several of these drugs remain FDA-approved for depression. Methylene blue is at least as dangerous as these very dangerous medications and is sold to an unsuspecting public, hearing promotions such as “three bottles for the price of two.”
When you take methylene blue, you are exposing yourself to the original lab-manufactured “psychiatric drug” from the 1890s that is so toxic to the brain and body and has so many bad interactions with other drugs and foods that even Big Pharma has not tried to get it approved by the FDA. Methylene blue can cause deadly serotonin syndromes and hypertensive crises, but much more commonly, it produces an artificial euphoria and manic reactions. The brain dysfunction that causes euphoria is very dangerous because it disinhibits people and is an early phase of the continuum of neurotoxicity that can lead to psychosis, mania, and violence. Ultimately, continued use of any such antidepressant can cause long-term chronic impairment of the brain and mind, and other organs of the body. All regularly used “antidepressants” act in this manner because they are modeled on and often derived from methylene blue.
Drugs.com Warns Healthcare Providers of Dangers of Methylene Blue, Even When Used Orally
Drugs.com8 provides several pages with long lists of adverse reactions from methylene blue. It is too long to include here. Then, in a section for “healthcare professionals,” it estimates the frequencies of some of the adverse effects. The top of the section specifically indicates that these reactions pertain to the compounded powders and tablets, which is how the drug is being dispensed as a liquid, powder, or tablet without prescriptions:
For healthcare professionals
Applies to methylene blue: compounding powder, injectable solution, intravenous solution, oral tablet.
Psychiatric
Common (1% to 10%): Anxiety
Frequency not reported: Confusional state, agitation
Nervous system
Very common (10% or more): Dysgeusia (20%) [taste decreased or lost], dizziness (16%), headache (10%), paresthesia [tingling, numbness or “pins and needles” on or under your skin]
Common (1% to 10%): Headache, paresthesia oral, dizziness postural
Frequency not reported: Serotonin syndrome (with concomitant use of serotonergic drugs), tremor, aphasia [disability comprehending or producing speech]
Cardiovascular adverse events
Common (1% to 10%): Chest pain, chest discomfort, presyncope, syncope
Frequency not reported: Cardiac arrhythmia, tachycardia, hypertension, hypotension, palpitations
Gastrointestinal
Very common (10% or more): Nausea (13%)
Common (1% to 10%): Vomiting, abdominal pain, diarrhea, hypoesthesia oral, oral discomfort
Frequency not reported: Feces discoloration (blue-green), dry mouth, flatulence, glossodynia [burning mouth syndrome], tongue eruption, thirst, oropharyngeal pain, blue colored saliva]
Immunology
Common (1% to 10%): Influenza-like illness, Influenza
Musculoskeletal
Very common (10% or more): Pain in extremity (84%)
Common (1% to 10%): Musculoskeletal pain, back pain, muscle spasms, chills, arthralgia
Frequency not reported: Serotonin syndrome, myalgia
Metabolic
Common (1% to 10%): Decreased appetite, limb discomfort
Frequency not reported: Local tissue necrosis at the injection site
Genitourinary
Very common (10% or more): Chromaturia (blue-green) (74%)
Frequency not reported: Dysuria [difficult or painful urination]
Hematologic
Common (1% to 10%): Ecchymosis [bruising]
Frequency not reported: Hemolytic anemia, hemolysis, methemoglobinemia, hemoglobin decreased, hyperbilirubinemia (in infants only)
Hypersensitivity
Frequency not reported: Anaphylaxis
Local [injection site]
Common (1% to 10%): Injection site pain, injection site discomfort
Frequency not reported: Infusion site extravasation, infusion site induration, infusion site pruritus, infusion site swelling, infusion site urticaria, peripheral swelling
Ocular
Frequency not reported: Mydriasis, eye pruritus, ocular hyperemia, vision blurred
Hepatic
Frequency not reported: Elevated liver enzymes [indicators of liver dysfunction]
Respiratory
Common (1% to 10%): Dyspnea [shortness of breath]
Frequency not reported: Dyspnea, tachypnea, hypoxia [loss of oxygen, potentially life-threatening],9 nasal congestion, rhinorrhea, sneezing
Other
Very common (10% or more): Feeling hot (17%), fever
Common (1% to 10%): Feeling cold, discomfort, catheter site pain
Frequency not reported: Genotoxicity [damage to the genetic information within a cell causing mutations, which may lead to cancer], fever, lack of effectiveness, interference with in-vivo monitoring devices, interference with laboratory tests
Dermatologic
Very common (10% or more): Skin discoloration (blue) (13%), hyperhidrosis (13%), sweating
Common (1% to 10%): Pallor, contact dermatitis, pruritus, cold sweat, erythema
Frequency not reported: Urticaria [hives], necrotic ulcer, papule, phototoxicity, rash (blue macules, severe burning pain)
The above is the complete list for “healthcare providers,”10 including some reactions from Short-term injection rather than ingestion. The frequencies of adverse effects are very high, which is typical of MAOIs, but surprising when there are few long-term exposures in regard to the accepted uses for methylene blue.
Remember, this list applies to the liquid, powder and tablet forms that are routinely on sale without prescriptions.
FDA Publishes Serious But Incomplete Warnings About Methylene Blue
The FDA has issued serious warnings about methylene blue, titled FDA Drug Safety Communication: Serious CNS reactions possible when methylene blue is given to patients taking certain psychiatric medications.11
Although these warnings are based on combining methylene blue with other antidepressants, it is a matter of degree, and all the adverse effects can be caused by methylene blue alone. The reports are mostly based on brief injections of methylene blue, commonly requiring a single dose. The FDA warns that methylene blue is a “potent” “monoamine oxidase inhibitor” and elaborates on safety measures to be taken after potential adverse events. It states:
The reported adverse events include the following: lethargy, confusion, delirium, agitation, aggression, obtundation, and coma. These symptoms were frequently accompanied by neurological symptoms, such as myoclonus, expressive aphasia, hypertonia, and seizures, or autonomic symptoms, such as pyrexia and elevated blood pressure.
The FDA notes the danger of an extreme serotonin syndrome caused by methylene blue in combination with other similar drugs:
It is believed that when methylene blue is given to patients taking serotonergic psychiatric medications, high levels of serotonin can build up in the brain, causing toxicity. This is referred to as Serotonin Syndrome. Signs and symptoms of Serotonin Syndrome include mental changes (confusion, hyperactivity, memory problems), muscle twitching, excessive sweating, and fever.
How the Brain Is Injured and then Injures Itself by Fighting Against Methylene Blue and All Psychoactive Substances
The direct injuries of neurotoxins on our complex brain are infinite. Innumerable research papers are published every year on how various psychoactive drugs, including psychiatric drugs, injure the brain on the cellular and biochemical level, and too often it is gross enough to be detected using sophisticated functional analyses as well as PET scans. Basically, any psychoactive substance that affects the brain and mind, even if it “feels good,” is poisoning the highest centers of the brain and harming or destroying multiple brain functions on a cellular and biochemical level. I have discussed this in many scientific articles and books, especially in great detail in my medical textbook, Brain-Disabling Treatments in Psychiatry, Second Edition.12
In that book, using the SSRI antidepressants as a model, I described at least three compensatory actions by the brain that go into action to inhibit the drug-induced excitatory neurotransmissions while adding new imbalances to the brain. First, when the brain senses the drug-induced pathological changes, the cells of origin of the particular monoamine transmitter stop producing it. Second, the receptors on the cells that receive the neurotransmission become less sensitive or die. And third, the transport mechanisms for removing serotonin from the synapse increase their power to remove the neurotransmitter.
These changes in the brain, forced on it by the neurotoxins, add to the harm from the drugs. In animal studies, these compensatory changes can persist long after the drug has been stopped. That is one cause of withdrawal reactions.
While I was able to unearth this research early in my career by simply looking for it in the scientific literature, it is practically a secret in the profession of psychiatry. Even professionals rarely learn about how the brain resists drugs because it is rarely taught in medical schools or residencies, and rarely mentioned in textbooks of medicine or psychiatry, which essentially promote drugs as part of the Psychopharmaceutical Complex.
How People Significantly Harmed by Methylene Blue, or Any Psychoactive Drug, Often Mistakenly Believe It is Helping Them
In my private practice, I regularly withdraw patients from psychiatric drugs with similar biochemistries to methylene blue. As the patients recover, they often realize for the first time how blunted they have become since starting on the drugs. I have characterized this lack of self-awareness about the neurotoxic effects of neurotoxic substances while under their influence as “medication spellbinding” or, more technically, medication anosognosia—the failure to identify one’s mental and emotional decline while taking psychiatric drugs. As I describe in my book, Psychiatric Drug Withdrawal, it derives from the dysfunction in the frontal lobes invariably produced by psychiatric drugs given at normal, effective doses. Medication spellbinding applies to all psychoactive substances, both medical and non-medical, and helps to explain why people continue to take harmful drugs.
Another reason many individuals stay on harmful drugs is that they become confused and discouraged by painful withdrawal symptoms, which definitely can occur with methylene blue (see below). Withdrawal effects often confuse patients, family members, or doctors because they can be misunderstood as proving the need for the drug when they, in fact, reinforce the need to get off the harmful drugs. Withdrawal symptoms prove that the drug is having a negative effect that is being covered up until the person tries to withdraw.
Both medication spellbinding and withdrawal are especially confusing to the person who is taking the medication, so even if methylene blue is “helping you,” you may be dead wrong.
The emotional insensitivity can last for a lifetime as long as the drugs are still taken. As I help patients carefully and gradually withdraw from the drugs, almost everyone becomes more able to reengage with their own inner life, with the lives of the people they love, and with every aspect of their own lives.13
The Brain-Disabling Principle of Psychiatric Drugs, including Methylene Blue
Methylene blue has so many destructive impacts on the body that it is beloved by researchers who imagine it will still someday prove to be a miracle drug in psychiatry, and even in neurology and elsewhere.14 This twisted thinking is the source of all psychiatric drugs — that by pouring neurotoxins into the brain, and disrupting its most basic processes, we are going to somehow cure “mental illnesses” by making the brain function better. This is what I have, for many decades, researched and called “the brain-disabling principle of psychiatric drugs.” It not only applies to neurotoxic psychiatric drugs, but more grossly to lobotomy and electroshock (ECT).
Poisoning the brain with neurotoxins, burning holes in it with psychosurgical electrodes, and traumatizing it into a coma with huge overdoses of electricity in ECT, would be simply ludicrous if were not the cause of tens of millions of deaths and untold billions of injured brains and minds, and the mainstay of psychiatry and the psychopharmaceutical industry.
I have researched and written about the “brain-disabling principle of psychiatric treatment” in many scientific articles and in easily available books, including the textbooks Brain-Disabling Treatments in Psychiatry: Drugs, Electroshock, and the Psychopharmaceutical Complex, second edition (2008) and Psychiatric Drug Withdrawal: A Guide for Prescribers, Therapists, Patients and their Families (2013), as well as in the popular book, Medication Madness: The Role of Psychiatric Drugs in Cases of Violence, Suicide and Crime (2008).
Marketing methylene blue as especially “pure” and “strong” may sound good, but since methylene blue is a neurotoxin in the same class as the oldest so-called anti-depressant, Monoamine Oxidase Inhibitors (MAOIs), purity and strength make it potentially far more dangerous.
Marketers may also claim the drug is being dispensed in small, safe doses, but that has no basis. First, people vary highly in how they react to low doses of neurotoxins. Second, if you are beginning to “feel good” or “energetic” or “highly focused” or “filled up with buoyancy and clarity,” your brain is already being made sick. It is being poisoned, and many poisons, especially those of a stimulant nature, make us feel good — and the better we feel the more our brain is being hyper-energized into a continuum of over-stimulation that can cause very bad judgement, disinhibition, anger and irritability, and eventually mania and violence, followed by crashing into depression and suicidality.
There are no drugs that interfere with your neurotransmitters without harming your brain and mind. Because psychoactive drugs cross the blood-brain-barrier, their effect is always widespread enough to reach the most elaborate or highest centers of your brain that control functions like love, reason, judgment, self-control, and overall sanity.
Methylene blue, which is considered a “potent” MAOI by the FDA, suppresses or breaks down the function of an enzyme called monoamine oxidase. The scientific process describes MAOI inhibitors as “degrading” the enzymes, making them ineffective in controlling these neurotransmitters, in effect unleashing four of the best-studied, most powerful, and stimulating neurotransmitters in the animal and human brain.
Monoamine oxidase is essential to the equilibrium system of the brain. It acts to inhibit at least four well-studied monoamine enzymes from becoming too active or energized: serotonin, dopamine, norepinephrine and epinephrine.
Imagine the danger. With your first dose of an MAOI drug, your control mechanism over four potentially stimulating or activating neurotransmitter systems is inhibited or abruptly disrupted in your brain. Yes, in a flash, it may seem good, great, or extraordinary, but at considerable potential cost in terms of injury to your brain, mind, and life.
This destructive process involved in destroying the monoamines in our brains is called “modulating” neurotransmitter systems by advocates of the MAOIs. In fact, these neurotoxic agents are vastly impairing the natural, existing modulation system in the brain by inhibiting or destroying monoamine oxidase. To this day, continuing with the SSRIs and the SNRIs, this is the primary mechanism of action for many or most psychiatric drugs, especially the antidepressants and stimulants.15
Cocaine is another drug that causes hyperactivation of these same four neurotransmitters—serotonin, dopamine, norepinephrine, and epinephrine.16 Another is methylphenidate (Ritalin, Focalin, and other names), and others are methamphetamine (rarely used in psychiatry) and amphetamine (often used as Adderall). Textbooks of pharmacology put all these stimulants into the same chapter about stimulants.
Serotonin Syndrome as a Cause of Brain Damage and Death
The worst adverse effect of methylene blue is death from serotonin syndrome — a state of extreme central and peripheral nervous system excitation that can be lethal. I have considerable experience with this potentially deadly and brain-damaging syndrome because it can also be caused by the so-called selective serotonin reuptake inhibitors (SSRIs) antidepressants, such as Prozac, Paxil, Zoloft, Lexapro and Celexa and the selective serotonin-norepinephrine reuptake inhibitors (SNRIs) including duloxetine (Cymbalta), venlafaxine (Effexor XR), and desvenlafaxine (Pristiq).
With MAOI antidepressants, the serotonin syndrome is a particular threat (along with malignant hypertension). The following is from the Parnate FDA Full Prescribing Information:17
Manifestations of the serotonin syndrome may include mental status changes (e.g., agitation, hallucinations, delirium, coma), autonomic instability (e.g., tachycardia, labile blood pressure, dizziness, diaphoresis, flushing, hyperthermia; with possible rapid fluctuations of vital signs), neuromuscular symptoms (e.g., tremor, rigidity, myoclonus, hyper-reflexia, incoordination), seizures, and/or gastrointestinal symptoms (e.g., nausea, vomiting, diarrhea). Fatal outcome of serotonin syndrome has been reported…
Many years ago, I had a new patient come to me, a sophisticated health professional in his thirties named John, who was receiving an SSRI from his psychiatrist and getting worse as the psychiatrist increased his dose. John’s more astute therapist noticed that John was having a bad reaction to his medication and made the referral to me. I could tell John was cognitively impaired and very anxious, and he seemed physically ill. He did not seem overstimulated or sedated, but he mentioned that he felt jumpy and stiff, and that when he crossed his knees on one occasion the night before, one of his legs jumped oddly.
I asked permission to give John a brief neurological examination — something most psychiatrists rarely or never do—and the first thing I did was to lightly tap one of his knees. Instantly, John’s entire body went into a spasm with arms and legs flexing uncontrollably. This was not a convulsion or seizure, but one enormous spasm of all his large muscles from over-stimulation.
Fortunately, I was able to arrange with John’s internist to admit him for examination and treatment on a medical ward — not a psychiatric ward — where my diagnosis was confirmed and he was quickly and safely given treatment for a serotonin syndrome. Because his psychiatrist had failed to diagnose him and continued his exposure to the SSRI antidepressant, John had a long physical recovery and wrestled with memory and concentration difficulties for years.
Serotonin syndrome can occur in varying degrees. Without going into a potentially lethal serotonin syndrome, you might have a fever, a sense that your mind is a little off, or feel your muscles stiffening. But if you had no idea that methylene blue was causing it, and if you then took more because you felt in more need of relief, your life would be at risk.
Hypertensive crises are another problem with MAOIs. They can become serious without being recognized if no one is taking blood pressure. If untreated, they can be fatal.
Recognition of the serotonin syndrome and hypertensive crises has greatly curtailed the use of MAOI antidepressants in psychiatry, making it more obviously egregious to spread them out into the community in the form of methylene blue with unlimited supplies and without any realistic warnings.
Documenting Adverse Reactions to the Oral Use of MAOIs Similar to Methylene Blue Through FDA Analyses of MAOI Antidepressants
Pages of adverse reactions are documented in the labels or Full Prescribing Information for MAOI antidepressants, including serotonin syndrome and hypertensive crises. Here are some especially relevant descriptions of adverse events for Parnate (tranylcypromine) tablets:18
Psychiatric disorders: excessive stimulation/overexcitement, manic symptoms/hypomania, agitation, insomnia, anxiety, confusion, disorientation, loss of libido Nervous system disorders: dizziness, restlessness/akathisia, akinesia, ataxia, myoclonic jerks, tremor, hyper-reflexia, muscle spasm, paresthesia, numbness, memory loss, sedation, drowsiness, dysgeusia, headaches (without blood pressure elevation)
Here are some warnings from the Nardil (MAOI) FDA Full Prescribing Information in the section on Adverse Drug Reactions:19
Common (1% to 10%): Anorgasmia, hypersomnia, hypomania, insomnia, sleep disturbances
Uncommon (0.1% to 1%): Agitation, behavioral changes, confusion, euphoria, frank psychosis, hallucinations, nervousness, vivid nightmares
Rare (0.01% to 0.1%): Acute anxiety reaction, delusional parasitosis, manic reaction, precipitation of schizophrenia, toxic delirium
Frequency not reported: suicidal behaviors, suicidal ideation
Withdrawal Problems with MAOIs
Making matters worse, after prolonged use over several weeks or a few months, withdrawal from drugs like methylene blue and all antidepressants can cause serious withdrawal reactions, and so stopping the drug requires cautious withdrawal.
Here are warnings from the Mayo Clinic about withdrawal or discontinuation symptoms from MAOIs:20
Stopping treatment with MAOIs
Talk with your healthcare professional before you stop taking an MAOI.
Typically, MAOIs are not habit-forming. But if you stop an MAOI suddenly, you’re more likely to have discontinuation symptoms. This is sometimes called discontinuation syndrome. These symptoms can include:
Restlessness, irritability, or anxiety.
Upset stomach.
Feelings of tingling or burning.
Flu-like symptoms, such as chills, sweating, feeling generally unwell, and muscle aches.
Trouble sleeping.
Sluggishness, tiredness, or sleepiness.
Headache.
Confusion.
Dizziness.
The Mayo Clinic warning on MAOIs continues:
You’ll likely need to wait two or more weeks after the use of MAOIs before starting other antidepressants. This will help you avoid serotonin syndrome, where you have dangerously high levels of serotonin. During those two weeks, continue food and beverage restrictions and don’t take medicine that can cause serious interactions with MAOIs.
Many Other Drugs and Even Foods Can Cause Fatal Adverse Interactions with Methylene Blue
The risk of enduring a serotonin syndrome — or most of the other adverse effects of methylene blue and other MAOIs — is that the risks vastly increase with accidental exposure to innumerable other drugs, including all those that stimulate any of the four neurotransmitter systems that are stimulated by methylene blue.
Anyone taking psychiatric drugs, opioids, and alcohol is at risk of a bad interaction. And because methylene blue is likely to be unknown to your own doctor, you need to tell him or her that it is a monoamine oxidase inhibitor (MAOI) like the older and relatively dangerous MAOI antidepressants. As mentioned earlier, these are phenelzine (Nardil), tranylcypromine (Parnate), selegiline (Eldpryl, Emsam, Zelapar), and isocarboxazid (Marplan). Even St. John’s Wort can interact negatively with MAOIs.21
Here’s a warning from Drugs.com that specifically addresses the vast numbers of dangerous drug interactions, specifically for methylene blue:
Many drugs can interact with methylene blue. Tell your doctor about all your current medicines and any you recently stopped using, especially: alfentanil, fentanyl; buspirone; digoxin, digitalis; dihydroergotamine, ergotamine; phenytoin; pimozide; quinidine; warfarin (Coumadin, Jantoven); an MAO inhibitor – isocarboxazid, linezolid, phenelzine, rasagiline, selegiline, tranylcypromine, and others; an “SSRI” antidepressant – citalopram, escitalopram, fluoxetine, paroxetine, sertraline, Prozac, Paxil, Zoloft, and others; an “SNRI” antidepressant – desvenlafaxine, duloxetine, levomilnacipran, milnacipran, venlafaxine, Effexor, Cymbalta, Pristiq, and others; other antidepressants – bupropion, clomipramine, mirtazapine; or medicine to prevent organ transplant rejection – cyclosporine, sirolimus, tacrolimus.”
Drug Facts and Comparisons was a pharmacology book I frequently used until it went online as an expensive business product. The last edition was in 2017. It had a special section on methylene blue.22 Going through three pages of fine print, I counted more than 100 dangerous drug interactions listed and many of those were for large numbers of drugs in a single category. Here is a selection of dangerous interactions listed alphabetically: Amphetamines, Analgesics (opioids), Antipsychotic agents, Blood glucose lowering agents, Cannabinoid-containing products, Cyclobenzaprine (Flexeril)’ Dextromethorphan (cough medicine), Epinephrine, Fentanyl, Hydrocodone, Levodopa, Methylphenidate, Potassium chloride, Reboxetine, Thiazide and Thiazide-like diuretics, Trazodone, Tricyclic antidepressants.
The current massive promotion and distribution of methylene blue is in many ways worse than the massive distribution of prescriptions. Methylene blue is promoted with incredibly unrealistic claims for cognitive improvement, high energy, and profound feelings of well-being — all of which are really danger signs of brain dysfunction from over-stimulation of four key neurotransmitters in the brain. In respect to methylene blue, there is little or no informed consent, and hardly anyone realizes they are taking a highly toxic neurotoxin at least as dangerous as the worst prescription antidepressants and worse than most.
Conclusion
Our freedom and health freedom movements are surprisingly involved in the promotion and use of methylene blue. Is this sudden prolific marketing and use of methylene blue one more aspect of the assault on our movements? I know that this definitely is not the intention of many who promote it. If anything, they are looking for relief from their strenuous efforts for truth and freedom.
Remember, all psychoactive drugs impair our higher mental functioning, easily and quickly rendering us unable to care about or defend our human rights or to make the best decisions on behalf of ourselves and others. That robs us of our own personal sovereignty and adds to the defenselessness of our society and nation against oppression. And further remember, you may be the last person to realize what happens to you under the “influence” of drugs, so pay attention to when trusted friends or family members tell you about the negative impact on your mind and behavior. When you are temporarily feeling your best, you may be suffering from a euphoria or “high” caused by drug-impaired brain function, and that can lead to mania, psychosis, violence, or suicide.
I began this effort to publicize the dangers of methylene blue in my regular guest hour slot on the Tamara Scott Show on Worldview TV, where her moral and ethical insights added greatly to my presentation.23 This May 6, 2025, video of the show may be a useful way for people to learn about the risks of methylene blue. In the closing remarks, my friend Tamara declared I had really dropped a bomb when I declared, “I think this is a CIA program,” and went on to explain how the CIA would want to destroy the Health Freedom Movement, and how the drug company Eli Lilly found a way to make tons of LSD and began giving huge amount to the CIA for its experiments on unwitting, involuntary people and also sold it into large crowds of Americans. The documentation is in an endnote from a CIA document from December 23, 2024, a book about the CIA and MKUltra, and from two of our radio interviews with a physician who survived CIA drug-involved abuses as a child.24
If you feel that your well-being is dependent on psychoactive drugs, except for the judicious use of prescribed opioids for pain of physical origin, you are probably taking your life in the wrong direction. The good feelings you are getting are a sign that the drug is actually interfering with your natural brain function and that your brain is being compelled to make compensatory changes that will harm your functioning as well. In fact, as a medical expert, I have found that “feeling great” after starting an antidepressant such as an MAOI, an SSRI, or an SNRI is often a signal of impending mania, depression, or delirium that can lead to suicide or violence.
Living a mentally and emotionally good life takes self-understanding, ethical principles, and conducting ourselves on the basis of reason, love, and devotion to higher ideals including a loving God. All psychoactive substances impair the highest human functions required for living life as best as possible and methylene blue is among the most dangerous.
Dare to trust in a Loving God
Express gratitude for your gifts and opportunities
Take responsibility at all times
Stand firmly for freedom
Become a source of love
Listen to the podcast on this story here: Emergency notification for methylene blue! It’s highly neurotoxic to your brain and mind
By Peter R. Breggin MD
Published first on AmericaOutLoud.news May 16-17, 2025
End Notes
1 All stimulants from caffeine to Ritalin (methylphenidate) and on to methamphetamine and cocaine, and including MAOIs, can produce subjective feelings of improved concentration or memory, and some short-term studies show a brief improvement. This is caused by obsessive-compulsive mental focusing and is driven by a narrowing of general awareness and judgment. No FDA-approved stimulants, for example, have been proven to help cognition or academic performance, and all harm the brain long-term. Here is as study that is negligent in its claims and its lack of warnings about methylene blue that may have encouraged the current epidemic use: https://psychiatryonline.org/doi/full/10.1176/appi.pn.2016.pp8a5 I have researched these issues in multiple scientific papers and books, including Brain-Disabling Treatments in Psychiatry: Drugs, Electroshock, and the Psychopharmaceutical Complex, second edition (2008). For an easily accessible, comprehensive look at stimulant drug effects, also see my free resource center on children and stimulant medications: https://breggin.com/Childrens-Resources-Center
2 Drug Safety Communication: Serious CNS reactions possible when methylene blue is given to patients taking certain psychiatric medications | FDA and FDA Drug Safety Communication: Updated information about the drug interaction between methylene blue and Drug Safety Podcasts > FDA Drug Safety Podcast for Healthcare Professionals: Updated information about the drug interaction between methylene blue and serotonergic psychiatric medications (methylthioninium chloride) and serotonergic psychiatric medications | FDA and much more comprehensive coverage of methylene blue adverse effects with special warnings for professionals can be found at Methylene Blue Monograph for Professionals – Drugs.com
3 Half_a_century_of_antidepressant_drugs_-20151101-21548-vmvosk-libre.pdf. Also see Methylene Blue: The Long and Winding Road From Stain to Brain: Part 2 – PubMed and Methylene Blue in the Treatment of Neuropsychiatric Disorders – PubMed; and Iproniazid | Antidepressant, Monoamine Oxidase Inhibitor & Mental Health | Britannica; Methylene Blue: The Long and Winding Road From Stain to Brain: Part 2 – PubMed; Monoaminergic neurotransmission: the history of the discovery of antidepressants from 1950s until today – PubMed. These cover the fascinating history of MAOIs and Methylene Blue.
4 The currently approved MAOI antidepressants are phenelzine (Nardil), tranylcypromine (Parnate), selegiline (Eldpryl, Emsam, Zelapar), and isocarboxazid (Marplan).
5 Breggin, Peter. “The Psychophysiology of Anxiety.” Journal of Nervous Mental Diseases, 139, 558-568, 1964 and Breggin, Peter. “The Sedative-like Effect of Epinephrine.” Archives of General Psychiatry, 12, 255-259, 1965.
6 Especial see these books by Peter Breggin: Brain-Disabling Treatments in Psychiatry: Drugs, Electroshock, and the Psychopharmaceutical Complex, second edition (2008). Springer Publishing Company; Medication Madness: The Role of Psychiatric Drugs in Cases of Violence, Suicide and Crime (2008). St. Martin’s Press; Psychiatric Drug Withdrawal: A Guide for Prescribers, Therapists, Patients and their Families (2013). Springer Publishing Company.
7 Microsoft Word – Peter-R-Breggin-MD-resume-121024.docx. For actual descriptions of many of my legal cases, see Medication Madness: The Role of Psychiatric Drugs in Cases of Violence, Suicide and Crime (2008) in the index under “cases” and for additional earlier cases, see Breggin, P. and Breggin, G. Talking Back to Prozac (1994) in the index under “Prozac case studies/testimony).”
8 https://www.drugs.com/sfx/methylene-blue-side-effects.html
9 According to Mayo Clinic, “Hypoxia is low levels of oxygen in your body tissues. It causes symptoms like confusion, restlessness, difficulty breathing, rapid heart rate, and bluish skin. Many chronic heart and lung conditions can put you at risk for hypoxia. Hypoxia can be life-threatening. If you are experiencing symptoms of hypoxia, call 911 or go to the nearest ER. Hypoxia: Causes, Symptoms, Tests, Diagnosis & Treatment
10 The order of the list of adverse effects has been changed to put some of special interest or relevance nearer the top, including psychiatry and neurology. The brackets contain my explanatory notes and the parentheses from the original.
12 The discussion of compensatory reactions is under the subheading “The Brain Resists the Impact of SSRIs, “ pp. 175-178) and “Causing Brain Dysfunction and Shrinkage,” pp. 178-182).
13 Especially see, P. Breggin. Psychiatric Drug Withdrawal: A Guide for Prescribers, Therapists, Patients and their Families (2013). Springer Publishing Company.
14 Methylene Blue: The Long and Winding Road From Stain to Brain: Part 2 – PubMed and Methylene Blue in the Treatment of Neuropsychiatric Disorders – PubMed
16 Epinephrine is often overlooked in scientific papers about cocaine, because there is less of it in the body than norepinephrine, but it is also activated by cocaine. Intravenous cocaine increases plasma epinephrine and norepinephrine in humans – ScienceDirect
17 PARNATE® (tranylcypromine) tablets, for oral use
18 PARNATE® (tranylcypromine) tablets, for oral use
19 Nardil Side Effects: Common, Severe, Long Term under the term adverse effects.
21 Monoamine oxidase inhibitors (MAOIs) – Mayo Clinic
22 Drug Facts and Comparisons, pp. 587-589, small print, double spaced. The subject heading is specifically for methylene blue. It is from the 2017 edition (its last book form).
23 https://worldviewtube.com/tv/video/medical-monday-tamara-scott-dr-peter-breggin-5
24 Here are some documents pertaining to CIA abuses using drugs: The book is Stephen Kinzer (2019). Poisoner in Chief: Sidney Gottlieb and the CIA Search for Mind Control, see its index for LSD as a start. The CIA document is CIA Behavior Control Experiments Focus of New Scholarly Collection | National Security Archive. Our interviews with Juliette Engel, MD, are
and
. The CIA document says that Eli Lilly may have donated the LSD but the book says the CIA paid them $400,000. For more about Eli Lilly, I was appointed by consortium of lawyers and confirmed by a federal judge to the single scientific expert on discovery from Eli Lilly in what was supposed to be innumerable trials eventually but Elli Lilly literally fixed the first trial, as determined by the Kentucky Supreme Court, and that dissuaded dozens of unwitting attorneys from continuing to pursue the cases or to take minimal settlements. It was only later that the Kentucky Supreme Court gave its opinion condemning the drug company and lawyers. See my book, Medication Madness, “The Infamous Wesbecker Case,” in Chapter 18: Drug Companies.
763 Likes∙
Discussion about this post
May 18Edited
Those of you who are describing your negative experiences with methylene blue in the comments below are providing a great service. Physicians and researchers often get their first inkling of a serious drug reaction from comments on the internet.
Roger Sterling, whose identity we cannot discover beyond his name, has inadvertently done us a great service by putting up an AI analysis of my methylene blue article. I have suspected that methylene blue is actually being pushed by the global predators who in fact control AI. I welcome people to review the attack on me and my article, and the strong defense of methylene blue. That AI would go to such an extreme to defend a severe neurotoxin, while attacking my very scientific analysis, which is also based on decades of clinical experience with these agents, confirms my initial grave concern that methylene blue is indeed a weapon directed against the health freedom movement and the freedom movement who are specifically over involved in promoting this and ultimately against the American population. It is time for us to all remain extremely alert for covert assaults against the health of our nation right at this moment when the Trump administration is conducting a MAHA campaign which in general, we support.